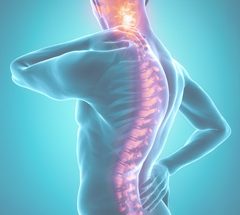
Neck Strains and Sprains
Mechanical neck pain can be caused by whiplash or injury or by the normal bad habits of our daily activities.
Neck pain is a common medical complaint, in large part due to our lifestyles. Awkward positions such as cradling the phone between the ear and shoulder, sitting in a chair that offers no support, or working at an ill-designed computer station can contribute to neck strain.
Many people also get neck pain from whiplash, which is a type of neck strain that may develop after an automobile accident when the head is suddenly and quickly forced forward and backward (excessive flexion and extension) during a rear-end collision. Other causes of whiplash include injuries during sports or biking. Although the pain can be severe, most episodes of acute neck pain are easily treated and improve with conservative care. There is a higher risk of future recurrences, so education about the condition is important to reduce this risk.
Causes of mechanical neck pain
Remarkably, only seven small vertebrae and an intricate system of soft tissues (muscles, tendons and ligaments) support the head and enable it to move in a wide range. The neck (or cervical spine) is the most mobile segment of the spine, but this mobility also makes it susceptible to injury.
Sprains and strains are soft tissue injuries. Soft tissues in the cervical spine include muscles, tendons and ligaments. Injury is sustained when these tissues are stressed beyond their normal limits. Degeneration with inflammation of motion segments of the spine such as discs and joints (such as facet joints) can also be causes of pain.
Symptoms
“Mechanical” means the pain is associated with certain movement or postures of the spine, which exerts stresses on specific pain generators of the spine. The pain intensity varies depending upon these mechanical factors. The distribution of pain in mechanical neck pain generally does not radiate past the shoulder. The initial pain may be so severe that the patient fears something is broken. At this point, many patients seek the advice of their physician.
Diagnosis
The physician will begin by taking a detailed history and physical exam and will want to assess if there may be a more serious condition related to the neck pain. The physician may order an X-ray, blood tests or more advanced imaging tests. An MRI may be considered if a more serious cause of back pain needs to be ruled out.
Treatment
Treatment is usually two-fold, including medications to relieve pain and muscle spasm and participation in a physical therapy program. The types of medications to relieve pain may include acetaminophen, non-steroidal anti-inflammatories, muscle relaxants, and occasionally opioids (narcotics).
Physical therapy incorporates therapeutic exercises, and modalities such as ultrasound, massage, heat or ice packs, and electrical stimulation. Therapeutic exercise programs begin slowly to acclimate the patient to stretching and strengthening routines. The patient is usually provided with a home exercise program to continue on a regular basis.
A strong and agile spine is one step toward preventing future injury. Exercises work to decrease inflammation, muscle spasm and pain.
Prevention
You can minimize stress on the neck by using proper posture and good body mechanics. Physical therapists teach patients how to develop ergonomically correct body mechanics in their everyday activities. Additionally, a work site ergonomic assessment can be very helpful.
A medical work-up by a spine physician may be necessary in order to rule out more serious causes of neck pain. Though frequently self-limiting, the condition often recurs. Physical therapy can be helpful to treat the acute pain. Perhaps even more importantly, therapy can also provide exercises to strengthen the core muscles that support the spine and educate about optimal body mechanics. In combination these measures reduce the risk of recurrences. A spine physician at Orthopedics International can assist with this common, but often challenging health care problem.