Cartilage Restoration
Cartilage is a specialized type of connective tissue. There are three main types of cartilage: hyaline (articular) cartilage, fibrocartilage, and elastic cartilage. Hyaline (articular) cartilage provides a smooth, white, glistening layer that covers the end of bones in a joint. The main functions of hyaline cartilage are to provide shock-absorbing properties and allow for a smooth, frictionless gliding surface in a joint.
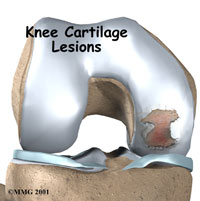
Cartilage injuries may present with pain, swelling, and/or locking if a fragment has separated in the joint. Hyaline cartilage has a limited capacity for healing due to its lack of blood supply. The surgical treatment options for cartilage damage are debridement (cleanup), microfracture to promote healing, and cartilage transplant. These procedures can be performed through a minimally invasive arthroscopic technique.
Microfracture
Microfracture is a technique used to treat full thickness cartilage defects with exposed bone. Hyaline (articular) cartilage has a limited capacity to regenerate and heal itself due to its lack of blood supply. This technique was developed as a way to stimulate the body to biologically repair cartilage injuries.
A minimally invasive arthroscopic technique is used to place microfracture holes into the exposed bone, which allows the release of blood and bone marrow contents into the cartilage defect. This activates a healing response and stimulates the production of a fibrocartilage layer to form over the exposed bone.
Microfracture is often used as a first treatment for small full thickness cartilage defects. The postoperative rehabilitation involves a period of limited weight bearing with crutches (4-6 weeks) and the use of a continuous passive motion machine (CPM). Large cartilage defects can be treated with microfracture or cartilage transplant.
Cartilage Transplant
Hyaline (articular) cartilage has a limited capacity to regenerate and heal itself due to its lack of blood supply. The only way to truly fill a cartilage defect with normal cartilage is through a cartilage transplant procedure. A number of cartilage transplant procedures have been developed which involve either transplanting cartilage and bone from one part of the knee to another (osteochondral transplant) or implanting new cartilage cells into the cartilage defect (autologous chondrocyte implantation).
Osteochondral Transplant
Osteochondral transplant procedures are designed to treat full thickness cartilage defects. They are known by a variety of names, including mosaicplasty and OATS procedure – a proprietary name that stands Osteochondral Autograft Transfer System. Osteochondral transplant involves harvesting a cylinder or plug of bone and overlying cartilage from an area in the knee that does not require cartilage and transplanting it into the cartilage defect. One or, sometimes, multiple plugs are transplanted to fill the cartilage defect completely. Large cartilage defects can be treated with allograft (cadaver) osteochondral grafts.
The advantage of this procedure is that the cartilage defect is filled with normal hyaline cartilage. The typical patient considered for this procedure is a young, active individual with a isolated traumatic cartilage injury. This procedure is performed through a minimally invasive arthroscopic technique or an open technique depending on the size and location of the lesion. The postoperative rehabilitation involves a period of limited weight bearing with crutches (6 weeks) and the use of a continuous passive motion machine (CPM).
Autologous Chondrocyte Implantation
This procedure was developed to fill the cartilage defect with more normal hyaline-like cartilage. It is sometimes referred to by its proprietary name – the Carticel procedure. It involves 2 separate operations. The first procedure is a short arthroscopic procedure where cartilage cells (chondrocytes) are harvested from a non-essential part of the knee. These cells are then grown (cultured) in a laboratory for 6-8 weeks. A second procedure is then performed to implant the chondrocytes into the cartilage defect under a small flap of tissue that is sewn into place. The flap of tissue holds the cells in place until they heal to the surrounding tissues and become hyaline cartilage. The second procedure is typically done as an open procedure. The result of this procedure is repair of the cartilage defect with nearly normal hyaline-like cartilage.
The typical patient considered for this procedure is a young, active individual with a isolated traumatic cartilage injury. The main disadvantage of this procedure is it requires two operations. The postoperative rehabilitation involves a period of non-weight bearing with crutches (8 weeks) and the use of a continuous passive motion machine (CPM).