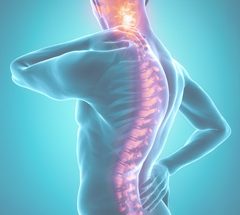
Sacroiliac Joint Injection
Learn about how the sacroiliac joint causes spinal pain, and the steps to getting a spinal injection that will provide relief and possibly help you avoid spine surgery.
The sacroiliac joint is formed by the connection between the sacrum of your spine and the ilium of the pelvis. If you are considering a sacroiliac joint injection, your doctor believes the joint may be a significant source of your spinal pain.
Why is a sacroiliac joint injection helpful?
First, the injection helps your physician confirm if the joint is the source of your pain. This can be done by measuring the amount of pain relief you feel after an injection of numbing medicine (anesthetic) into the joint.
In combination with the anesthetic, the injection can include a time-released steroid, which may prolong the relief of pain for several weeks. During this time of relief, your doctor may prescribe other treatments such as physical therapy.
What will happen to me during the procedure?
You will lie on your stomach for this procedure, with pillows positioned for optimal comfort. After the lower back area is prepped with special soap, numbing medicine will be injected in a small area of skin, which will sting for a few seconds. Next, a small gauge needle will be guided by X-ray into the joint. Contrast dye may need to be injected to ensure that the medicine flows correctly and not into a blood vessel. A small amount of numbing medicine and anti-inflammatory steroid will then be injected slowly into the joint and the needle will be removed.
What are the possible side effects of the injection?
- Bruising
- Temporary dizziness
- Temporary numbness
- Muscle ache from the needle insertion
- Infection (rare)
- Spinal cord or brain injury (extremely rare)
What should I do after the procedure?
Immediately afterwards, you may be given an injection report form, which will help you to monitor your pain levels after the procedure. Your physician will review this with you before you depart the clinic. The healthcare provider who referred you for the injection will assess the outcome of the procedure with you to determine the future course of your treatment.
Your doctor may refer you to a physical therapist or chiropractor right after the procedure while the numbing medicine is active and over the next few weeks while the steroid is working.
We prefer that you have a ride home, and if you do, you can leave right after the procedure if you feel normal. If you do not have a ride home and have not had any oral or IV sedating medicine, you can drive yourself home if, after being observed for 30 minutes after the injection, you do not develop any neurological symptoms.
General instructions before and after the injection:
- Do not eat for six hours before the procedure.
- Take your routine medicines before the procedure (such as high blood pressure and diabetes medicines). Do not take aspirin and all anti-inflammatory medicines such as Motrin® (ibuprofen), Aleve® (naproxen), Relafen® (nabumetone), or Daypro® (oxaprozin). These should be stopped five days before the procedure and can be restarted the day after the procedure. Unless directed otherwise by your physician, you may take other forms of pain medication (e.g., acetaminophen, narcotics).
- Unless you and your healthcare provider decide otherwise, do not take your regular pain medicine the day of the procedure, but you can restart itafter the procedure, if needed.
- If you are on Coumadin® (warfirin) or heparin, you must call our office to determine how long these medications should be stopped before the procedure and whether a blood draw is necessary. Typically, you will stop taking Coumadin for four days prior to the injection.
- If your procedure has a diagnostic purpose, we discourage the use of sedating or pain medication at the time of the procedure, as this may alter your perceptions of pain that are not related to the injection. If you receive any sedating or narcotic medication, you will need to have someone drive you home. You may return to your current activity level the next day, including returning to work.
- If you are an insulin-dependent diabetic, let your injection doctor know. Your insulin dose may be adjusted depending upon the time of day your injection is scheduled. After the procedure, your blood sugar may be temporarily elevated for a few days due to the steroid.
Because this is a non-urgent medical procedure, it is important that you do not have an acute infectious illness at the time of the spinal injection. If you are concerned about your fitness for the injection, please call your healthcare provider.